For as long as he can remember, Steve Chappell felt isolated from the world. Even among friends there seemed some chasm separating him from meaningful human connection. The despair manifested in his body, pulsing into excruciating headaches that made it feel like his eyes would pop out. From the time he was a child, he struggled to get out of bed.
“It’s almost like I needed a training manual to be myself,” he says, “but I didn’t have one.”
Depression may have run in his family, but Chappell—an only child raised by a single, widowed mother—lacked a frame of reference. It took years of hospital visits before a doctor diagnosed him with a major depressive disorder, giving him a name for what ailed him.
But it also marked the beginning of a three-decade struggle to treat the disorder, which sucked the joy out of life, and, at times, sent him to the brink of suicide. Medications—Prozac, Paxil and Zoloft, to name a few of the 13 he has tried—made him nauseous, sometimes violently ill.
“The psychotropic drug thing did not work for me,” says Chappell, a Silicon Valley data scientist who runs his own company. “I can tell you, it had the benefit of ruining two marriages.”
Last year, he hit bottom.
To save his third marriage, Chappell considered more extreme measures, namely shock therapy or a brain implant, before turning to a novel, apparently safer alternative: a magnetic helmet.
According to Dr. Saad Shakir, the San Jose-based neuropsychiatrist who treated Chappell, electromagnetic therapy is the best available treatment with the fewest side effects.
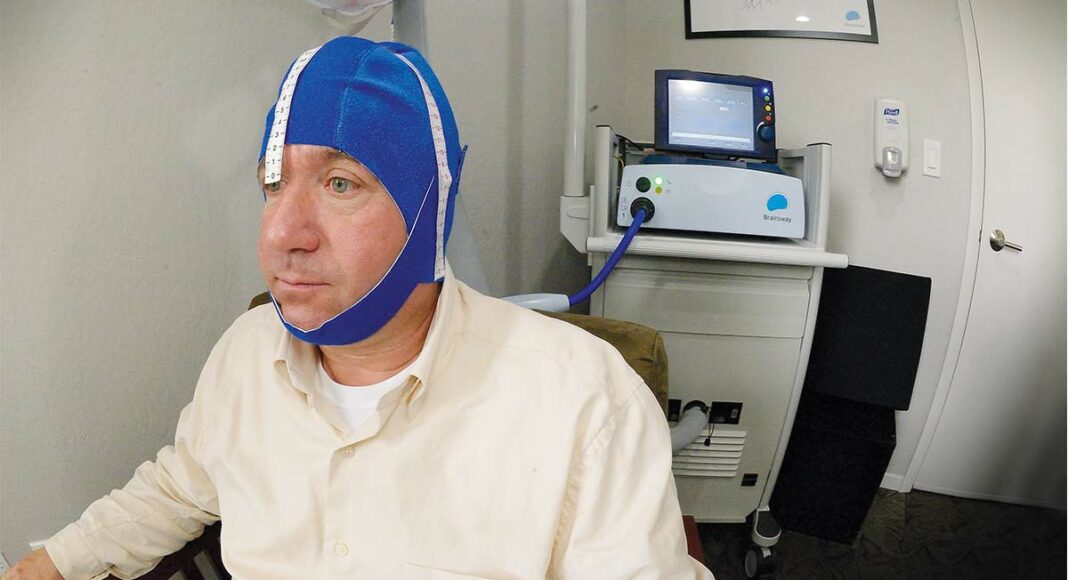
Called deep transcranial magnetic stimulation (TMS), the technology involves placing a cushioned helmet over a patient’s head while a machine delivers electromagnetic pulses to affected parts of the brain.
In 2007, the U.S. Food and Drug Administration approved the treatment for patients resistant to depression medications and talk therapy. According to the Journal of the American Medical Association, some 15 million Americans suffer from a major depressive disorder, but more than one-third fail to respond to antidepressants. A tenth—Chappell among them—have a genetic immunity or can’t stomach the drugs because of the side effects.
Three years ago, the FDA signed off on a new variation of the magnetic pulse treatment developed by Israeli company Brainsway. Called deep TMS, the machine generates a powerful magnetic field that travels a few centimeters through the scalp and skull and into the prefrontal cortex. The magnetic field changes the electrical activity of neurons, temporarily altering the way brain cells communicate. Unlike electroshock therapy, in which patients get zapped by seizure-triggering electrodes affixed directly on the scalp, TMS targets specific regions of the brain.
Brain neurons respond to stimulation in a perpetual balancing act between excitement and inhibition. Too much inhibition can lead to depression. Too much excitement can induce autism and seizures.
TMS treatment has shown some promise for neuropsychiatric conditions that seem to involve dysfunctioning brain circuits, including epilepsy, depression, obsessive-compulsive disorder, and, though the evidence is still thin, schizophrenia. It has also been used to treat people with autism, attention-deficit disorders, tremors, addiction, bipolar disorder, chronic pain and stroke.
“At first it was a little jarring,” Chappell says from a couch in Shakir’s sunlit office. “It feels mildly like a very small electrocution. Your face locks or twitches, some people get teary eyed.”
“Some patients describe it like a miniature jackhammer,” Shakir chimes in. “Or a woodpecker.”
The breakthrough for Chappell came this spring, halfway through the second week of treatment. For the first time in three decades, he says, his head cleared. About a month in, he felt calm, upbeat.
“The fog had lifted,” he says. “Things felt much sharper. I was smiling and laughing, which had been so hard for me. That became almost every day as the treatment progressed.”
For Chappell, TMS dispelled the need for antidepressants. Still, he keeps a dose of “rescue medication” just in case and undergoes cognitive behavioral therapy to address negative thoughts.
“It’s not a cure-all,” Shakir says of TMS. “But it’s transformational for the right patients.”
Though American doctors have spent decades testing magnetic therapies for various mood disorders, it wasn’t until federal approval in the new millennium that Shakir took up the cause. Once the FDA gave it the green light, he signed on as a provider and founded Silicon Valley TMS, one of 600 such centers nationwide and one of 11 in Northern California.
Still, questions persist about how many patients could benefit from TMS, which requires daily office visits for six weeks and maintenance sessions beyond that. Because it’s so new, there’s also a dearth of research on the long-term effects.
No one has figured out how to account for the placebo effect, in which patients feel better because they believe in the treatment. That would require building a fake TMS machine, and the electric charge that induces muscle twitching has proved a challenge to replicate.
Cost has been another barrier, with TMS running from $10,000 to $12,000 for a series of sessions and often not covered by insurance. Until recently, Shakir says, patients paid out-of-pocket at his for-profit clinic.
In the past few years, Kaiser, UnitedHealth, and Blue Cross have come on board. A few months ago, Cygna agreed to cover TMS. The American Psychiatric Association advises TMS for people who have tried one to four medications with little to no effect. But there’s no set standard for determining how a patient qualifies for the treatment.
“We’re trying to change that by raising the profile,” says Jon Miller, a retired Air Force veteran and TMS patient. As a pilot, Miller says, he lived in the shadows with his illness, which took a toll on his body and personal relationships.
Miller, who has been getting treatment from Shakir, sees TMS as an alternative to the “‘Band-Aid” approach of prescription pills for mentally ill vets.
Chappell says having the option of a non-pharmaceutical treatment gives him hope: “For each of us who have suffered for as long as we have, there is always a time where you go, ‘Enough, I shouldn’t be here any longer.’ That’s life threatening. You have to give people hope that they can get better.”
.New Brain Therapy Treats Depression